Integrated Home Care (ADI) is a key service to provide continuity of care for frail, chronic and post-acute patients directly at home. Increasing demand, an aging population and greater clinical complexity make it increasingly necessary to use limited resources efficiently. Operationally, ADI requires complex and interdependent daily decisions:
- assign nurses to patients
- Plan rounds (home tours)
- Manage fleet and vehicles, coordinating time windows, clinical priorities, and continuity of care
Managing this process manually or with static rules easily leads to inefficient routes, unbalanced loads, and difficulty in adapting to unforeseen events. Thus, a quantitative and data-driven approach is needed to jointly optimize routing and allocation of personnel and vehicles while maintaining high service quality. The implementation was developed in the context of a major ASST (>1.1 Mln population) having two locations for territorial management of the rapidly expanding ADI service.
Methodological approach
Step 1: Integrated modeling of assignment and routing
The ADI service is formalized as an integrated problem of:
- Nurse-patient assignment,
- Route planning with time constraints (visit windows).
The operating day is described through: location of patients, duration of services, time windows, skills required; resources through: shifts, vehicle availability, organizational constraints. This makes a craft-managed process measurable and governable.
Step 2: Optimization and scenario analysis for operational and strategic decisions
Based on the formalization, an optimization model is developed that:
- Minimizes travel time/distances,
- Balances the load between operators,
- Respects constraints and priorities.
The model, powered by real data, enables both day-to-day planning and scenario analysis (changes in demand, resources or fleet) to support decisions on sizing and organization.
Results
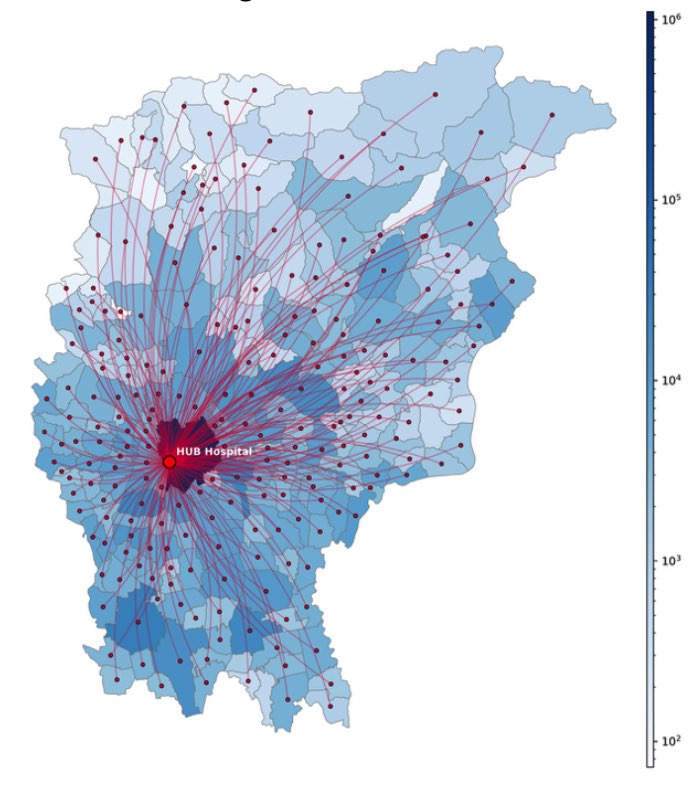
Reduced travel time
More efficient routes, fewer total kilometers (-12%) and better vehicle utilization.
Improved workload balance
More equitable distribution of patients among nurses, reducing overload and increasing organizational sustainability.
Increased service capacity with equal resources
More daily visits possible with the same number of nurses and vehicles due to more efficient scheduling (+8%-10%).
Increased operational resilience
Ability to re-plan in case of emergencies or unforeseen events (absences, clinical changes) while maintaining adherence to time windows.





