When service demand is variable and resources are limited, the risk of congestion grows rapidly: waiting times increase, intake capacity is reduced, and cascading inefficiencies are generated. The COVID-19 pandemic has amplified these dynamics, making clear the need for more integrated and coordinated solutions to manage peak influx and overflow of patients.
In this context, we proposed a centralized patient reallocation strategy focused on non-urgent cases. The idea is to take advantage of demand-capacity imbalances between facilities: when a hospital is saturated, some of the load can be redirected to less congested facilities, improving the distribution of patients throughout the system and reducing overall congestion.
The implementation was developed in a network of 4 emergency rooms affiliated with a single ASST that have an annual number of accesses exceeding 100,000.
Methodological strategy
Step 1 – Stochastic Optimization Model
Development of a stochastic model to optimize the reallocation of nonurgent patients under uncertainty scenarios, with objectives of:
- Minimize the overall time in the system (waiting + handling)
- Balancing demand and capacity between hospitals/clinics
Step 2 – Pooling (patient grouping) and fairness criteria
Introduction of patient pooling strategies and fairness constraints to ensure reallocation:
- flexible (adaptable to peaks)
- fair (avoiding making patients wait beyond reasonable time intervals),
Results
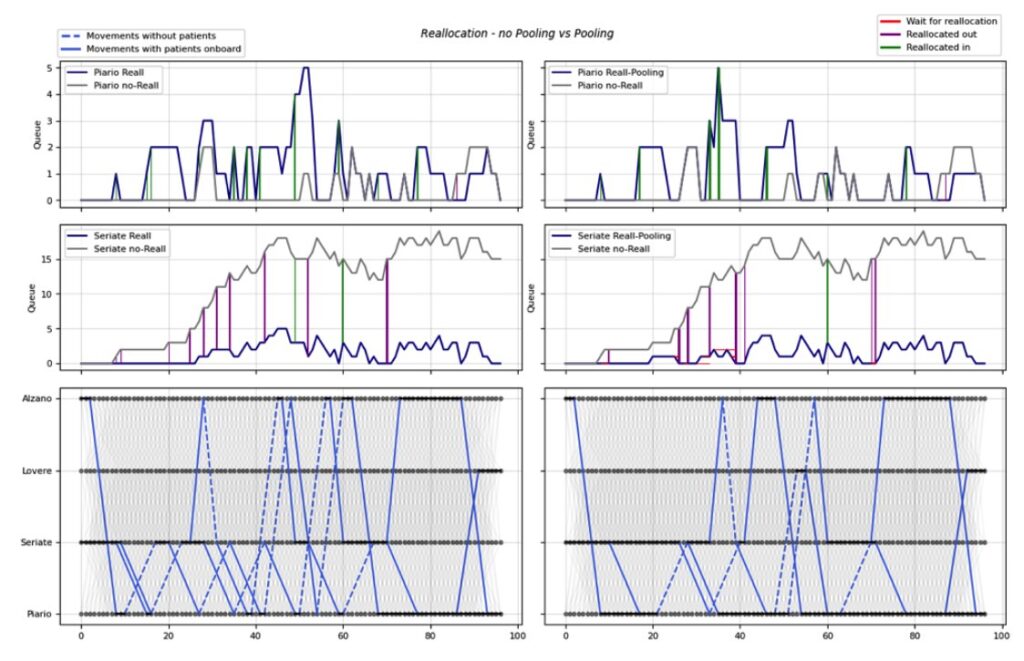
Better flow management
The on-demand approach reduces wait times by 25-30%, accelerating access to care and increasing throughput.
Optimizing “fleet”/transfers
Pooling strategy increases the number of reallocated patients on average, reducing fleet costs by 5-10%.
Greater stability in resource planning
Consistent routing strategy reduces waiting time by about 10 percent, making resource allocation more predictable and facilitating optimal fleet sizing.





