Ensuring continuous, quality nursing coverage is essential to hospital operations. However, shift planning is complicated by three recurring factors: need for 24/7 coverage, staff shortages, and constant pressure on cost containment. In traditional models, often based on manual planning or static rules, typical inefficiencies occur: over-coverage in some time slots (costs and unnecessary extra hours), under-coverage in others (clinical-operational risk and worsening patient experience), staff stress and burnout, resulting in turnover and absenteeism. Responding to variable demand for care (daily and weekly) requires a dynamic, data-driven approach capable of systematically adjusting coverage levels to actual need.
We have implemented an optimization system that supports the definition of staffing levels and the generation of individual shifts, with the goal of improving coverage, sustainability, and operating costs.
The model is designed for:
- Align nursing coverage with expected demand (and its variability)
- Reduce overtime and inefficiencies
- Improve balance and quality of allocations for staff
The implementation was developed in a medium to large, complex, multidisciplinary hospital setting with heterogeneous clinical-organizational constraints and a need for continuous coverage.
Methodological approach
Step 1 – Defining staffing levels (Robust optimization)
A “robust” optimization model determines optimal staffing levels taking into account uncertainty in patient demand, avoiding fragile solutions that work only “under ideal conditions.”
Step 2 – Individual Shift Generation (Mixed integer programming)
A mathematical programming model builds individual shifts and assignments respecting operational and organizational constraints, including:
- shifts and time slots
- allocations for staff in training
- tutor/support pairings
Results
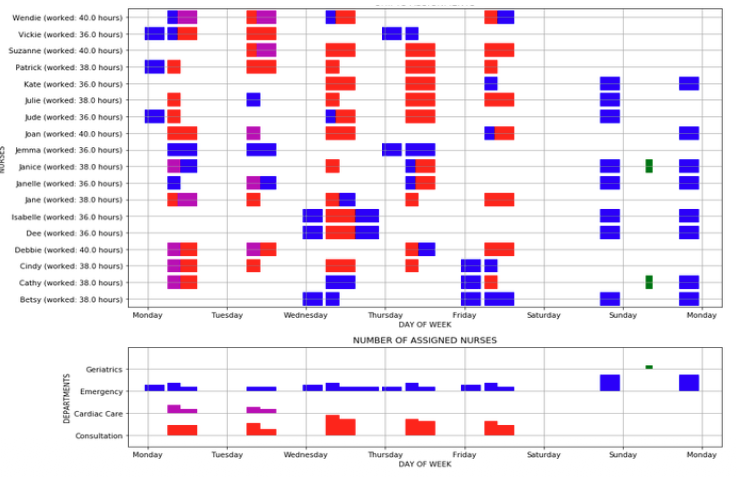
The introduction of the system has produced measurable benefits on service quality, staff experience and costs:
- Improved continuity of care coverage: Coverage more consistent and aligned with fluctuations in demand, with fewer critical issues related to understaffing.
- Increased staff satisfaction: More balanced and predictable shifts, reducing unbalanced load and burnout risk.
- Reduction in operating costs: Reduced overall costs through more efficient use of resources and less use of overtime.
A total cost reduction of 6-8% was observed in one implementation, preventing under-coverage.





